Patien Info
BENIGN PROSTATE HYPERPLASIA
BPH is benign prostatic hyperplasia, a noncancerous enlargement of the prostate that restricts the flow of urine from the bladder. If you are over 50 and have this condition, you are not alone. BPH affects millions of men worldwide.
Some BPH symptoms include:
- The need to urinate more often, especially at night
- Sudden sensation of incomplete emptying of the bladder
- Weak urine stream
- Need to strain or push bladder when beginning to urinate
- Frequent trips to the bathroom
-
Your doctor can easily screen for BPH by performing simple tests such as blood and urine tests.
What is BPH? Benign prostatic hyperplasia (BPH) with associated lower urinary tract symptoms (LUTS) is a common medical condition in the aging male. The incidence has been estimated to increase
from 50% among men between the ages of 50 and 60 years, to 90% for men older than 80 years of age. In 2016, it is estimated that up to 3 million men in the UK have lower urinary tract symptoms
suggestive of BPH. Traditionally the options have included making life-style changes for mild symptoms as well as medication and surgical procedures such as TURP or laser prostatectomy for men with
more severe symptoms or complications of prostate enlargement such as urinary infections or a complete stoppage (urinary retention).
What other treatment options are available?
Life-style changes and reassurance For men with concerns about prostate cancer and mild symptoms reassurance and advice regarding food and drinks is usually all that is required. This “watch and
wait” approach is employed for many men diagnosed with BPH. Treatment usually occurs once the symptoms of bladder outlet obstruction and bladder irritability interfere significantly with quality of
life. Traditionally, the primary objective of treatment has been to alleviate bothersome LUTS that result from prostatic enlargement.
Medication For many men, medications such as alpha blockers are the first line approach to control mild-tomoderate symptoms of BPH. These symptoms include frequent urination and getting
up at night as well as a deterioration in the flow of urine often with hesitancy and sometimes with a feeling of incomplete emptying. Choosing the correct medical treatment for BPH symptoms is often
complex and ever changing.
Issues Many men begin medical therapy but have: Inadequate or short-lived improvement in their symptoms and quality of life Undesirable side-effects that lead to discontinuation such as light
headedness and sexual problems
Increasingly, men do not want to commit to lifetime pharmaceutical treatment, particularly as they are
often taking other medication and there can be concerns relating to interactions between tablets. Remembering to take the tablets can also be an issue.
The most economical way of treating troublesome symptoms due to BPH is still not entirely clear but many men take medication for several years before going on to have surgery. Increasingly minimally
invasive surgical treatments are being offered to men with moderate symptoms, a reluctance to take/continue medication and a desire to return to normal activities quickly.
Minimally Invasive Procedures: At the present time there are other options. The results with Transurethral microwave thermotherapy (TUMT) and Transurethral needle ablation using radiofrequency
thermotherapy (TUNA) are at best modest and prostatic stents continue to cause problems.
Endoscopic surgery The removal of prostate tissue is called a prostatectomy and when there is benign (non cancerous) prostate tissue causing a blockage the central component of the prostate is
removed one way or another, in order to allow urine to flow more easily from the bladder.
For men with severe BPH symptoms including retention of urine, Transurethral resection of the prostate (TURP) has been the gold standard for a long time but increasingly men are looking at the
alternatives which include laser enucleation (Holmium laser) or vaporization (PVP using the 180W greenlight laser). These laser technologies remove prostate tissue by different means.
With all surgical procedures there are complications, side effects and risks as outlined below. Bachmann A, Hindley R et al – The Goliath Study, Eur Urol 2013 (a study which Basingstoke participated
in) demonstrated that the percentage of unplanned readmission rates following a TURP procedure was 13.5%.
The other recognised side effects are listed below:
Retrograde ejaculation (dry ejaculation) Erectile dysfunction (impotence) Urethral strictures or scarring Bleeding (occasionally requiring a transfusion) Urinary infection (UTI)
There are also other issues including a Hospital stay of several days (usually 3 days after TURP) and increasingly during the winter months, operations are cancelled due to lack of beds.
It is often 6 weeks before patients can return to normal activities and regular exercise.
Drug Therapy Evaluation
If you can answer yes to any of the questions below, you may want to discuss the REZUM Therapy with your urologist:
- Are you tired of taking daily medication?
- Do you sometimes forget to take your daily medication?
- Do you suffer from low energy, dizziness, or loss of libido?
- Has your drug therapy become less effective over time?
- Have you experienced swelling of the feet, breasts or lips while on drug therapy?
- Are you concerned about the interaction between your various medications? REZUM Therapy as an Alternative to Drugs
- Are you currently taking Flomax®, Proscar®, Cardura®, Hytrin® or Avodart® for your enlarged prostate?
- Are you frustrated with the sexual side effects often associated with medications prescribed for BPH?
- Have you considered discontinuing treatment or seeking help elsewhere because you're not satisfied with drug therapy?
- Are you aware of your alternatives?
- REZUM may be right for you
REZŪM ( Water Vapor Ablation of Prostate)
This booklet has been provided to help answer the questions you may have with regards to your enlarged prostate and the Rezūm procedure that is being offered to you. It explains what Rezūm is, what treatment options are available, as well as what can happen if you choose to undergo a Rezūm procedure. We will ask you to sign the consent form before the procedure if you decide to go ahead with surgery.
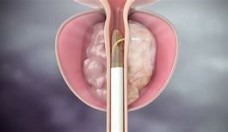
What is Rezūm? Rezūm is a method by which steam energy is used to ablate (or remove) the particular part of the prostate that enlarges and causes symptoms due to BPH. Specific technical information is explained below.
This system consists of a portable radiofrequency (RF) generator and delivery device that is introduced into the body via the urethra (transurethral approach) and guided by direct
visualization through a telescopic lens placed within the delivery device.
RF energy from the generator is applied to an inductive coil in the delivery device to heat up a controlled amount of water outside of the body, converting the water into vapour or steam. The
thermal energy created outside the body is delivered into the prostate tissue through a tiny needle with emitter holes to ablate the targeted obstructive prostate tissue that causes BPH. The
procedure takes approximately 3 - 7 minutes and can be performed in a Day Surgery setting. No RF energy is delivered into the body.
Throughout the insertion of the device and during the treatment saline (salty water) is running to help ensure better views and to prevent the urethra from overheating.
The generator has a number of safety features to ensure proper heating and thermal ablation of the targeted prostate tissue, while protecting the urethra during treatment. Thermocouples in the
delivery device monitor temperatures to ensure consistent delivery of thermal energy into the ablation region. The length of the vapour needle is fixed and the operator controls all functions
of the device. Placement of the vapour needle within the prostate is done under direct visualization through the telescopic lens, which is in the urethra inside the prostate.
The Rezūm System is intended to relieve the symptoms of obstruction and prostate tissue associated with BPH and is indicated for men with prostatic urethra lengths >2 .0 cm and prostate volumes
>20 cm3. The Rezūm System also is indicated for treatment of prostates with a median lobe or elevated central zone tissue.
What approvals does Rezūm have? The Rezūm System received CE Mark on 8th July 2013 and FDA clearance for use in the USA on 27th August 2015. Rezūm has NICE approval, under IPAG625.
What evidence of the benefits of Rezūm are available? There have been several clinical studies undertaken on the benefits of the Rezūm System and we can give you details if you would like to review
them. What happens next? You will be offered a date for the procedure and also for a pre-operative assessment if a general anesthetic is going to be used. If you have not already done a flow
test, this will be performed as well as completing the questionnaires. If you are on blood thinners, you may be asked to stop taking them for a period prior to your treatment. Treatment day You will
have been given a time to attend the hospital. Even though the procedure only takes a few minutes, you will probably be at the hospital some time before and after the procedure, again depending on
the anesthetic used. It is very likely that you will be discharged home the same day. You will sign consent forms and an example is attached. The treatment About an hour before, you will be given
some strong painkillers as well as some antibiotics which you will continue at home. You will then be accompanied to theatre where the procedure will take place. If you are having a general
anesthetic you will be sent to sleep. The majority of men will be awake for the procedure. Antibiotics will be given directly into your vein. Local anesthetic will then be administered around the
prostate gland with the use of an ultrasound probe via the back passage. This may feel a bit uncomfortable, but the more relaxed you are the easier it will be. The Rezūm equipment is then passed
through the urethra using plenty of anesthetic gel, which may momentarily sting. After a quick inspection of the bladder, the treatment will begin. On completion a catheter will be left within your
bladder for a few days prior to voiding as the prostate readjusts to the treatment and the swelling subsides. An antibiotic and pain killing suppository will
be inserted into your rectum at the end. When can I go home? After your procedure, you will be reviewed by a member of the urology team who will discuss the
operation, any specific requirements for you at home and a plan for your aftercare. A date will be given to you as when to return for the catheter removal as well as the care required whilst at home.
It is normal to have some pain or discomfort after operations, and we advise you on painkillers to help keep it under control. Return to work as you feel comfortable depending on your job. If in
doubt please check with your surgeon and obtain a certificate, before you are discharged
When you attend for catheter removal, please try to arrive with a full bladder so that you stay will be as short as possible. The tube will be removed and then when you are ready you will be asked
to void into the flow machine and the bladder scanner will detect any remaining volume of urine. If the nurse is happy with the results you will be discharged. If there are any problems you may
require a further period of catheterisation or be taught intermittent self catheterisation.
Within a few days you will be able to resume normal activities and should notice improvements within 2 weeks, although it may be 3 months before the full benefit is evident. Blood may be visible in
the urine and ejaculation fluid When can I resume sexual activity? We recommend you avoid ejaculation for 6-8 weeks following the procedure.
UROLIFT ( PROSTATE PULL)
The Urolift® procedure involves passing a telescope through your urethra (waterpipe), and putting two to four implants into your prostate to pull the obstructing tissue away from your urethra • It is designed to improve your urinary flow without the need for burning or removing any prostate tissue • You do not usually need to have a catheter put in after this procedure • Sexual side-effects such as retrograde (dry) ejaculation or erectile dysfunction (impotence) are very rare • In a small number of men who have this surgery, further treatment may be needed at a later stage
The main benefits of this procedure, compared with other surgical treatments for prostate enlargement, are:
• a short stay in hospital; • a minimally-invasive (minor) procedure; and • no sexual side-effects such as retrograde (dry) ejaculation or erectile dysfunction (impotence).
Your urologist can tell you whether the size and shape of your prostate means that this procedure is suitable for you, but it cannot be used in all men with prostate enlargement.
This can be done under local or General anaesthetic and is a Day Procedure
Not All Prostate are Suitable for this Procedure
BRACHYTHERAPY
What is Brachytherapy?
Brachytherapy is recognised as an alternative to both radical surgery and standard external beam radiotherapy.
Prostate Brachytherapy is a form of radiation treatment that is used for localised prostate cancer. The term Brachy is derived from the Greek word meaning “near.” During a Brachytherapy treatment, radioactive seed sources are placed directly inside the prostate gland. The radiation dose is delivered very near the cancer, greatly limiting the amount of radiation that is absorbed by other parts of the body. This allows for a higher dose of radiation to be given than is possible with external beam radiotherapy.
Brachytherapy is a short procedure, usually requiring only one night’s stay in hospital. Patients are usually able to resume their normal daily activities very quickly after having this treatment.
Who can receive the treatment?
If your cancer is localised to your prostate gland, and can be treated with surgery, you are likely to be eligible for Brachytherapy. Brachytherapy works well for prostate cancer when the cancer is small and fully contained within the prostate gland.
If you are over the age of 70, your doctor may recommend that you be treated using either external beam radiotherapy or active monitoring, instead of surgery. If your doctor feels that you should not have surgery because of your age, you may still be eligible for Brachytherapy treatments. Brachytherapy is suitable for patients of all ages and is usually recommended for individuals who have a life expectancy of 10 years or more.
Your cancer specialist may decide that you are not eligible for Brachytherapy if you have a very large prostate gland and/or severe urinary symptoms. However, these can be safely managed with medications so that you can still receive Brachytherapy.
Initial Assessment for suitability for Brachytherapy
An initial consultation is carried out by both a Consultant Urologist and an Oncologist. Your Consultant will review the stage and grade of your cancer during this consultation. Several tests will also be done, including a scan to assess your bladder emptying, and a flowmeter test to assess your urinary flow. An Ultrasound scan of your prostate gland will also be completed.
If your Consultant decides that you are ready to start Brachytherapy treatment, an appointment for your treatment will be arranged for you. You may need to take medications to shrink your prostate and improve your urinary flow before you can have your first treatment. If so, your general practitioner will be advised to prescribe these medications.
What is a volume study?
A volume study is an ultrasound assessment that is used to determine the size and shape of the prostate. A volume study is usually done one to two weeks prior to the first Brachytherapy treatment, and helps the doctor to decide the number of radioactive seeds that will be needed for a Brachytherapy treatment. An ultrasound probe is placed in the rectum and serial ultrasound scan pictures are taken to assess shape and size of the prostate.
The procedure lasts for about half an hour, and is performed at the Rivers Hospital.
The procedure
You will be given a list of instructions to follow to prepare your bowel for your Brachytherapy treatment. A clean, empty rectum is needed on the day of your treatment so that good images of your prostate can be obtained using the ultrasound rectal probe.
The doctor will insert an ultrasound probe into your rectum (please see the diagram below). Serial images of your prostate will be recorded. Using these images, a 3-D brachytherapy treatment plan is created by an advanced computer planning system. This allows the doctor to see how many radioactive seeds will be needed, and to see where the seeds should be placed. During the treatment, the placement of seeds is monitored using X-ray Imaging, Ultrasound Imaging, and the computer planning system. By monitoring your treatment in this way, the doctor can ensure greater than 99% coverage of the cancer with radiation.
Needles containing the radioactive seeds will be inserted through your perineum [the area of skin beneath your scrotum] into your prostate (please see the diagram below). You will be given a general anaesthetic, or sometimes, an epidural anaesthetic, before these needles are inserted. The seeds are then deposited into the prostate, in the areas and quantities that your doctor has determined will most effectively treat your cancer.
After your treatment, you will be taken to the recovery room until the effects of the anaesthetic have worn off. You will then be returned to your room and stay hospital for one night. You will have a catheter inserted into your bladder to allow you to pass urine. You will also be given painkillers, as some slight discomfort is expected following the treatment. The Urologist or Radiotherapist may visit you in your room after your treatment.
While you are in hospital, you will not be placed in special isolation because almost all of the radiation from the treatment is absorbed by your prostate. The radiation level outside your body is safe for others, letting you resume your normal activities immediately after leaving the hospital.
The morning after the treatment, the catheter will be taken out and you will be allowed to go home as soon as you are able to pass urine. You will be prescribed medications to reduce swelling of your prostate.
|
|
|
|